COVID at-home Tests
Beginning January 15, 2022, at-home over-the-counter COVID-19 diagnostic tests authorized by the U.S. Food and Drug Administration (FDA) will be covered at no cost for WHA members (with limits on reimbursement as outlined by regulatory guidance, below).
Members have the following options for coverage and obtaining OTC at-home COVID-19 test kits:
- You can order up to 4-free rapid tests from the federal government at covidtests.gov
- Pay $0 at a preferred network pharmacy: Visit the pharmacy counter at a Rite Aid, Sam’s Club, Walgreens or Walmart Pharmacy and present your member ID card and ask to have your OTC at-home COVID-19 test kits submitted to your plan for coverage.
- Purchase a kit and then submit an online form for reimbursement: WHA members who purchase an FDA-approved COVID-19 diagnostic test on or after January 15, 2022, will be able to submit a reimbursement request form, with a scanned receipt, for the cost paid up to $12 per diagnostic test. This is only available to active WHA members, per FDA EUA guidance, with a limit of eight (8) tests per calendar month. Members will need to save receipts and attest/sign that tests will be used for personal use, will not be used for employment purposes, and will not be resold. Reimbursement is only for FDA-approved, at-home test kits (see a full list here).
- A Claim Reimbursement webpage is available through the WHA Pharmacy partner OptumRx at https://covidtest.optumrx.com/covid-test-reimbursement and will accept receipts dated on or after January 15, 2022.
- Kit purchased; then print and mail in a paper reimbursement form. You can print a claims form link then mail it in. WHA will reimburse up to $12 per test.
- Note: CalPERS members should check details on the CalPERS webpage.
Q: Is there a limit to how many tests will be covered?
A: Yes. Eligible plan members can get up to 8 individual tests per month.
Q: Which COVID-19 tests are covered?
A: Coverage includes OTC at-home test kits authorized by the Food and Drug Administration (FDA).
Visit Coronavirus Disease (COVID-19) webpage for the latest updates or reach out to the pharmacy department: Pharmacy@westernhealth.com
Prescription Medication Update
WHA is closely monitoring drug shortages listed on the FDA website. A member's pharmacy has up-to-date information from their suppliers regarding drug shortages. If your WHA patient/member is affected by a drug shortage, have the member contact their pharmacy so they can assist. If for some reason the member is unable to access their current supply of prescription medications, or if they need an additional supply, they can call WHA Member Services to request an early refill at 888.563.2250. Note: CalPERS members should contact OptumRx at 855.505.8110 for early refill requests.
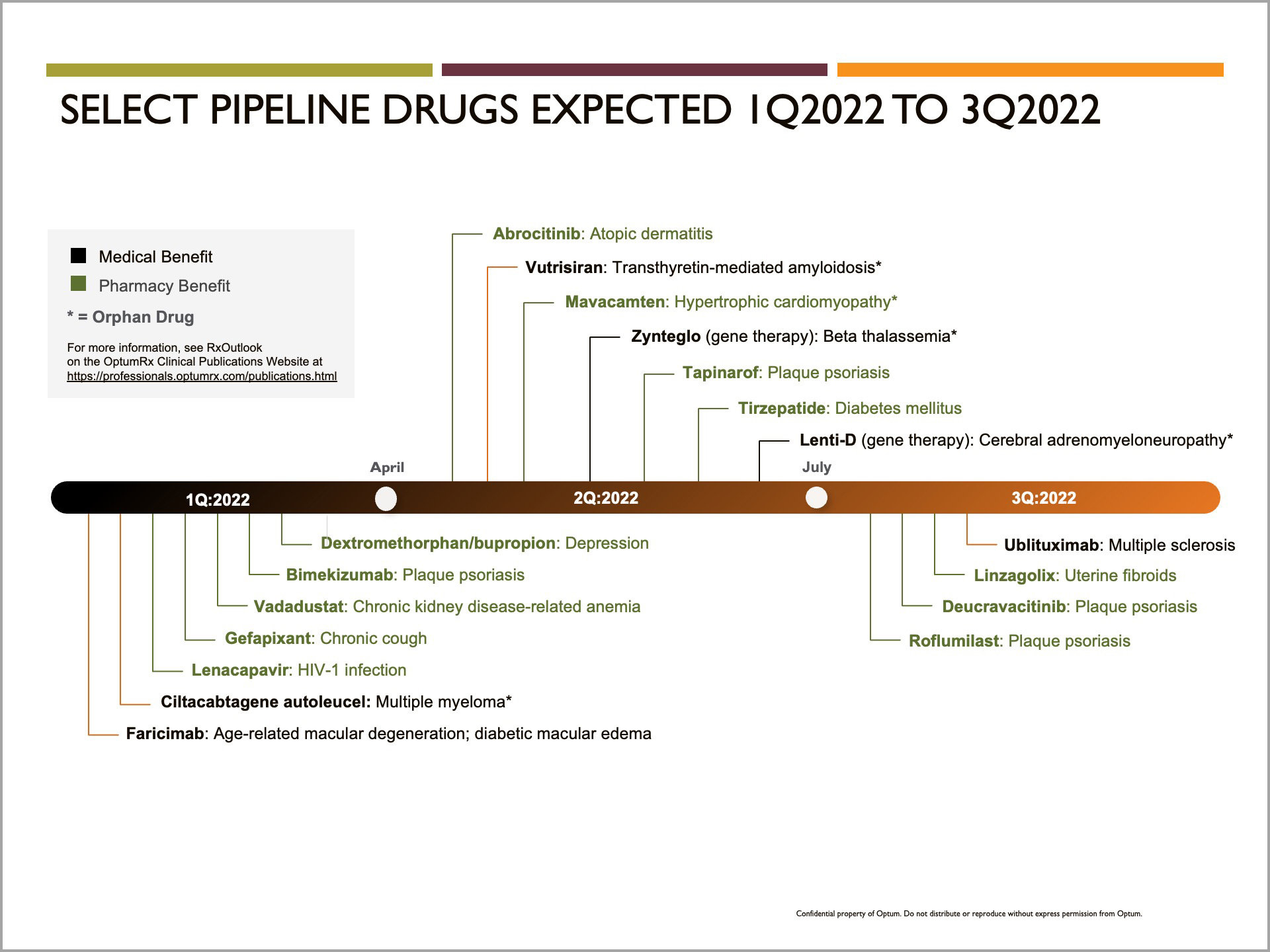
Pharmacy Drug Pipeline Review (1Q’22)
WHA continues to monitor pipeline drug launches including generic products, this remains a large focus during our quarterly P&T meeting. During our 1Q2022 meeting, we reviewed select pipeline drugs expected for 1Q2022 through 3Q2022, in addition to generic launched slated for 2022. Information below has been provided by our PBM partner.
.jpeg)
.jpeg)
